Blog
Burning Sensation on Genitals: Causes & Care
A burning sensation on the genitals can be uncomfortable, distressing, and sometimes alarming. It may occur suddenly or gradually and can affect both men and women. While mild irritation may resolve on its own, persistent or severe burning should not be ignored.
Burning sensation on the genitals may signal an underlying infection, skin condition, or sexually transmitted disease (STD). Understanding the possible causes, associated symptoms, and when to seek medical evaluation can help prevent complications and provide peace of mind.
What Does a Burning Sensation on the Genitals Feel Like?
Genital burning can feel uncomfortable and alarming, especially when it appears suddenly or without a clear cause. It may range from mild irritation to persistent discomfort that may be accompanied by:
- Stinging or irritation
- Rawness or sensitivity
- Warmth or heat in the genital area
- Pain during urination
- Discomfort during sexual activity
The sensation may affect the vulva, vagina, penis, scrotum, groin, or around the anus. It can occur constantly or only during specific activities such as urination or intercourse.
Common Causes of Burning Sensation on the Genitals
A burning sensation in the genital area can be caused by conditions ranging from mild irritation to infections requiring treatment. Because symptoms may resemble early signs of an STD/STI or other genital issues, identifying the exact cause is important for proper care. Below are the most common causes in both men and women:
1. Yeast Infection (Fungal Infection)
Yeast infections are a common cause of genital burning, especially in women. They occur when there is an overgrowth of Candida fungus. Symptoms may include:
- Intense itching
- Thick white discharge
- Redness and swelling
- Burning during urination or intercourse
Men can also develop yeast infections, particularly under the foreskin, leading to redness, irritation, and discomfort.
2. Sexually Transmitted Infections (STIs)
Several STDs can cause genital burning, particularly when urinating or during sexual contact. These include:
- Chlamydia
- Gonorrhea
- Genital herpes
- Trichomoniasis
- Syphilis
Herpes may cause painful blisters that burn or sting. Chlamydia and gonorrhea often cause burning during urination along with abnormal discharge. Some infections may initially present with mild symptoms, making regular screening important if risk factors exist.
3. Urinary Tract Infection (UTI)
UTIs commonly cause a burning sensation during urination. Women are more prone due to anatomical factors. Additional symptoms may include:
- Frequent urge to urinate
- Cloudy or strong-smelling urine
- Lower abdominal discomfort
Prompt treatment prevents the infection from spreading to the kidneys. Early care also reduces discomfort, lowers the risk of complications, and helps prevent recurrent urinary infections.

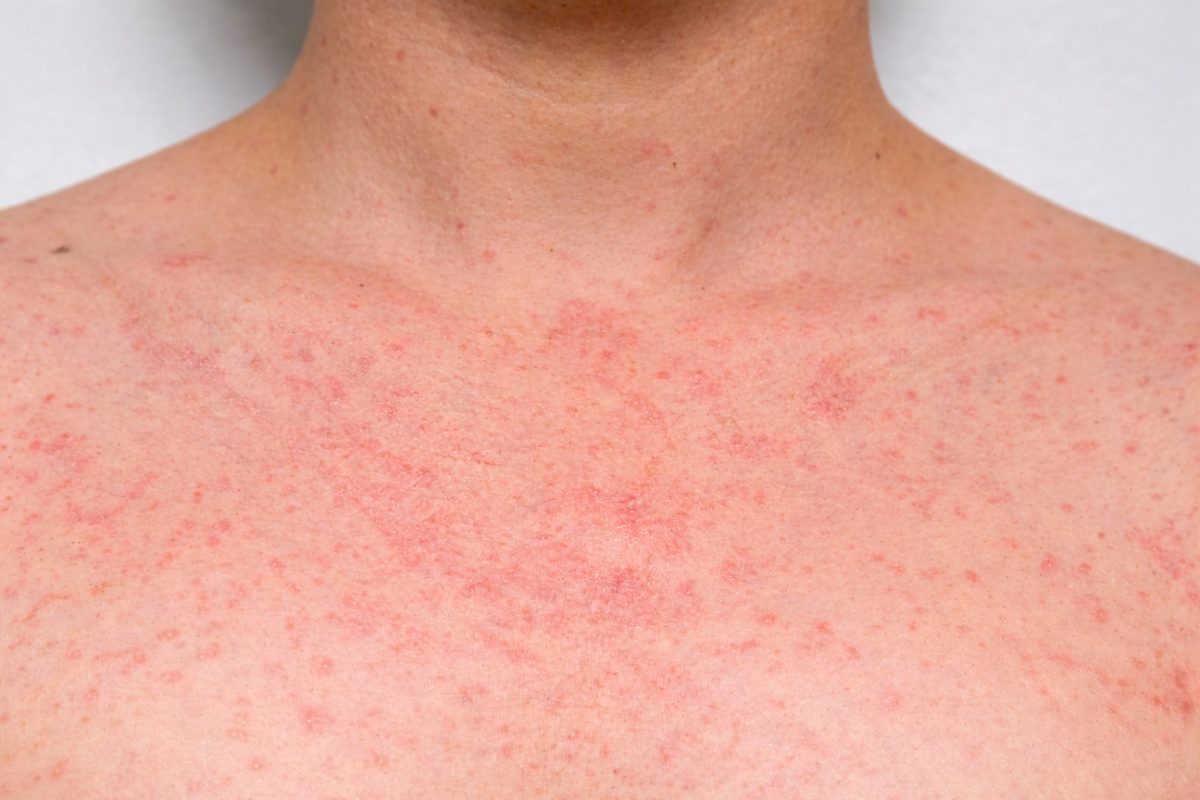
4. Skin Irritation or Contact Dermatitis
Genital skin is sensitive and can react to a variety of external irritants and internal changes. Because the skin in this area is thinner and more delicate than other parts of the body, it is more prone to inflammation and discomfort. Genital skin is sensitive and can react to:
- Scented soaps
- Intimate washes
- Laundry detergents
- Tight clothing
- Latex condoms
This irritation can cause redness, dryness, and burning without infection. Removing the trigger often improves symptoms.
5. Bacterial Vaginosis (BV)
In women, bacterial vaginosis occurs when the natural balance of vaginal bacteria is disrupted. Symptoms may include:
- Thin greyish discharge
- Fishy odor
- Mild burning or irritation
Although not always sexually transmitted, it is more common in sexually active individuals. This is because increased sexual activity may expose the genital area to a higher risk of bacterial imbalance, irritation, or infection.
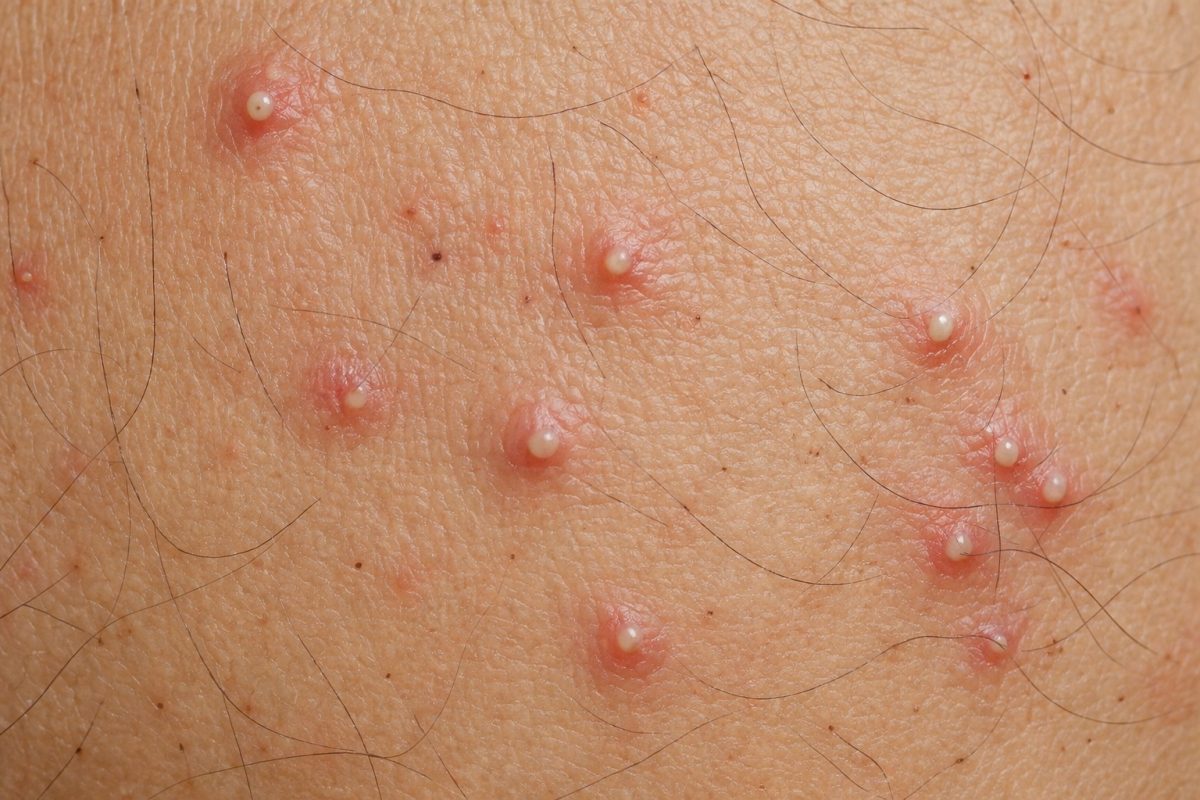
6. Genital Herpes
Genital herpes causes clusters of painful blisters or ulcers that may burn before they appear. The burning sensation may occur as an early warning sign known as a “prodrome.” Outbreaks can be triggered by stress, illness, or weakened immunity.
7. Hormonal Changes
Hormonal fluctuations during menopause, postpartum recovery, or breastfeeding may cause vaginal dryness and thinning of tissues. This can result in burning, especially during intercourse or urination.
When Burning May Indicate a More Serious Condition
While mild irritation may resolve on its own, persistent or worsening burning should not be ignored. It may indicate an underlying infection or STD that requires prompt treatment, and delaying evaluation can increase the risk of complications. Seek medical evaluation if you experience:
- Persistent burning lasting more than a few days
- Genital sores or ulcers
- Abnormal discharge
- Fever
- Pelvic pain
- Pain during sex
- A partner diagnosed with an STD
Early assessment ensures proper diagnosis and prevents complications such as pelvic inflammatory disease (PID) or recurrent infections.
How Is Genital Burning Diagnosed?
Diagnosis begins with a detailed medical history and physical examination to understand your symptoms, sexual history, and possible risk factors. This step helps narrow down potential causes and ensures that appropriate tests are performed. Your doctor may:
- Perform a genital or pelvic examination
- Take swabs for infection testing
- Conduct urine tests
- Recommend STD and STI screening
- Order blood tests if needed
Testing may include screening for chlamydia, gonorrhea, syphilis, HIV, herpes, or trichomoniasis, depending on symptoms and risk factors. Accurate diagnosis is essential because treatments differ significantly depending on the cause.
Treatment Options
Treatment depends on the underlying condition, which is why proper diagnosis is essential before starting any medication. The approach varies depending on whether the cause is infectious, irritant-related, or hormonal. Early and appropriate treatment not only relieves discomfort but also prevents complications and recurrence.
For Infections
Bacterial STDs and UTIs are treated with antibiotics, yeast infections with antifungal medication, and genital herpes with antiviral therapy. Prompt treatment relieves symptoms and reduces transmission risk. Completing the full course of prescribed medication is essential to ensure effective recovery and prevent recurrence.
For Irritation or Allergic Reactions
Avoiding irritants, switching to fragrance-free products, and wearing breathable cotton underwear may help. Topical soothing creams may be recommended if appropriate. Maintaining proper genital hygiene and keeping the area dry can also reduce irritation and support healing.
For Hormonal Causes
Vaginal moisturisers or lubricants may reduce dryness-related burning. Hormone therapy may be considered in certain cases under medical supervision. Regular follow-up with a healthcare provider ensures that treatment is safe, effective, and tailored to individual needs.
Avoid self-diagnosis or relying solely on over-the-counter products without confirmation, as this may delay appropriate care and allow underlying infections to worsen.
When to See a Doctor
You should seek medical care if burning persists, worsens, or is accompanied by genital discharge, ulcers, fever, pelvic pain, or bleeding. Testing is especially important if you are sexually active or unsure about possible STD exposure. Early evaluation provides reassurance, prevents complications, and ensures effective treatment.

Take Genital Symptoms Seriously
A burning sensation in the genitals is not something to ignore. While it may result from minor irritation, it can also indicate infections or other medical conditions that require professional care. Addressing symptoms early protects your sexual health and overall well-being.
Dr Chong Clinic provides confidential consultation, comprehensive STD screening, and personalised treatment in a professional and supportive environment. If you are experiencing genital burning or related symptoms, booking an appointment ensures clarity, proper care, and peace of mind.
Frequently Asked Questions (FAQs)
1. Is a burning sensation on the genitals always caused by an STD?
No, genital burning is not always caused by a sexually transmitted disease. It may result from yeast infections, urinary tract infections, skin irritation, or hormonal changes. However, testing is recommended if risk factors are present.
2. Can stress cause a burning sensation in the genital area?
Stress does not directly cause burning, but it can weaken immunity and trigger conditions like herpes or eczema. Anxiety may also increase sensitivity to discomfort.
3. How long does genital burning usually last?
The duration depends on the cause. Mild irritation may resolve within a few days. Infections usually improve after starting appropriate treatment. Persistent symptoms lasting more than a week should be evaluated.
4. Can I treat genital burning at home?
If symptoms are mild and due to irritation, avoiding triggers may help. However, self-treatment without diagnosis is not recommended, especially if discharge, sores, fever, or ongoing discomfort are present.
*All images used in this article are AI-generated.