Blog
Can Oral Sex Cause STDs? Risks & Prevention
Oral sex is often seen as the “safer” option compared with vaginal or anal sex. Because there is no penetration in the usual sense, many people assume the risk is very low, or even negligible. That assumption is common, but it is not entirely accurate.
While the risk may be lower for some infections, oral sex is not risk-free. Sexually transmitted diseases (STDs) and infections can still be passed through oral contact, even when there are no obvious symptoms. This is why it is important to understand what can spread this way, how it happens, and what steps actually reduce the risk.
How STDs Spread Through Oral Sex
Oral sex involves contact between the mouth and the genitals or anus. Infection can spread when bacteria or viruses enter the body through delicate tissues in the mouth or throat, especially if there are small cuts, sores, or inflamed gums. This can happen through:
- Small cuts or sores in the mouth
- Inflamed or bleeding gums
- The lining of the throat
- Contact with infected skin or bodily fluids
Even without ejaculation, transmission can still occur. Pre-ejaculatory fluid, vaginal secretions, and skin-to-skin contact may be enough, depending on the infection involved.
STDs That Can Be Transmitted Through Oral Sex
Several common STDs can spread through oral sex. In many cases, a person may not realise they are infected, which is why transmission can happen without warning.
1. Gonorrhea
Gonorrhoea can infect the throat after oral sex. This is often called pharyngeal gonorrhoea. Some people have no symptoms at all, while others may notice a sore throat, redness, or swollen glands. Because throat infection is easy to miss, someone may continue passing it on without knowing.
2. Chlamydia
Chlamydia can also infect the throat, although it is less common than genital infection. When it does happen, symptoms are often mild or absent. That makes testing important after possible exposure, especially if a partner has tested positive.
3. Syphilis
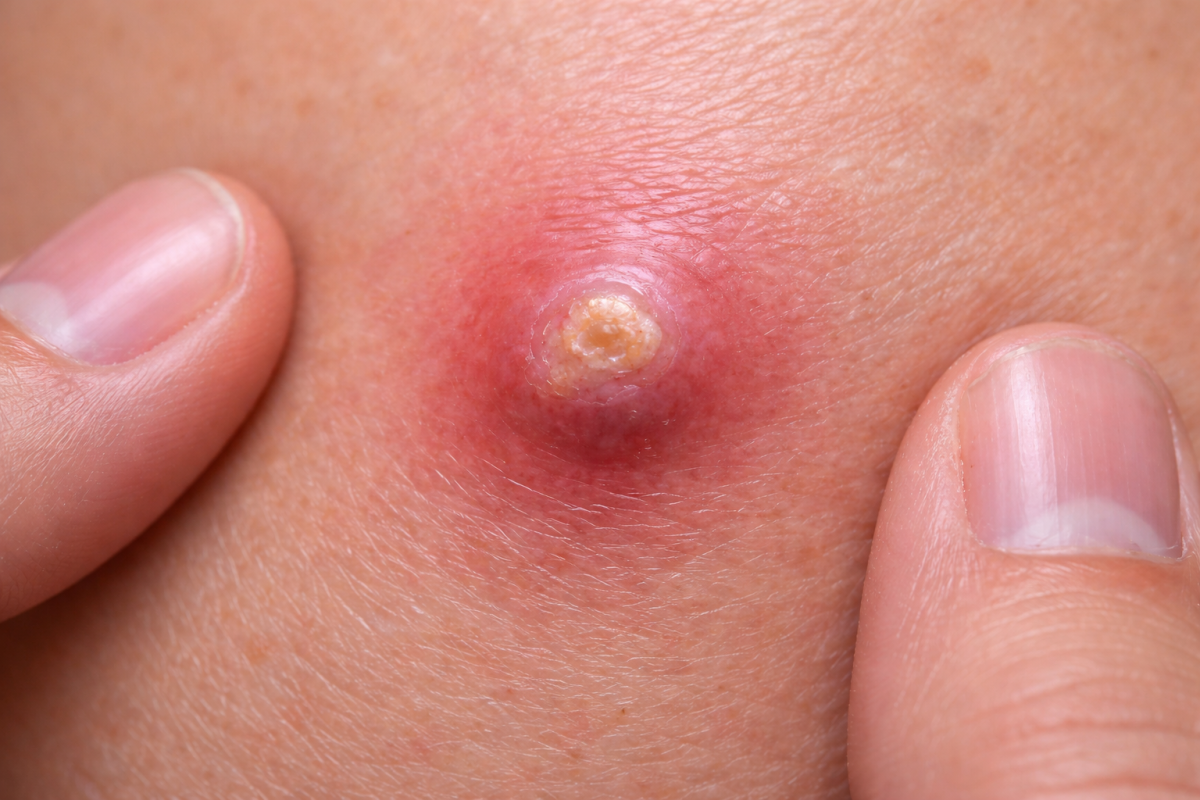
Syphilis spreads through direct contact with sores. These sores can appear on the genitals, anus, lips, or inside the mouth. Sometimes they are painless, which makes them easy to miss. A person can become infected through oral sex even if the sore seems small or harmless.
4. Genital Herpes (HSV-1 and HSV-2)
Herpes can spread in both directions. A person with oral herpes can pass the virus to a partner’s genitals during oral sex, and genital herpes can also infect the mouth. What makes herpes especially tricky is that it can spread even when there are no visible sores.
5. Human Papillomavirus (HPV)
HPV spreads through close skin contact, including oral sex. Some strains are low risk and may cause warts, while others are linked to cancers of the cervix, anus, penis, and throat. Many people with HPV have no symptoms, so it can go unnoticed for a long time.
6. HIV
The risk of HIV transmission through oral sex is lower than with vaginal or anal sex, but it is not zero. The risk becomes higher if there are mouth sores, bleeding gums, ejaculation in the mouth, or a high viral load in the infected partner. Although this route is less common, it is still medically recognised.
7. Hepatitis B
Hepatitis B can spread through infected bodily fluids. It is less commonly passed through oral sex than some other infections, but the risk is not absent, especially if blood exposure is involved. Vaccination offers strong protection.
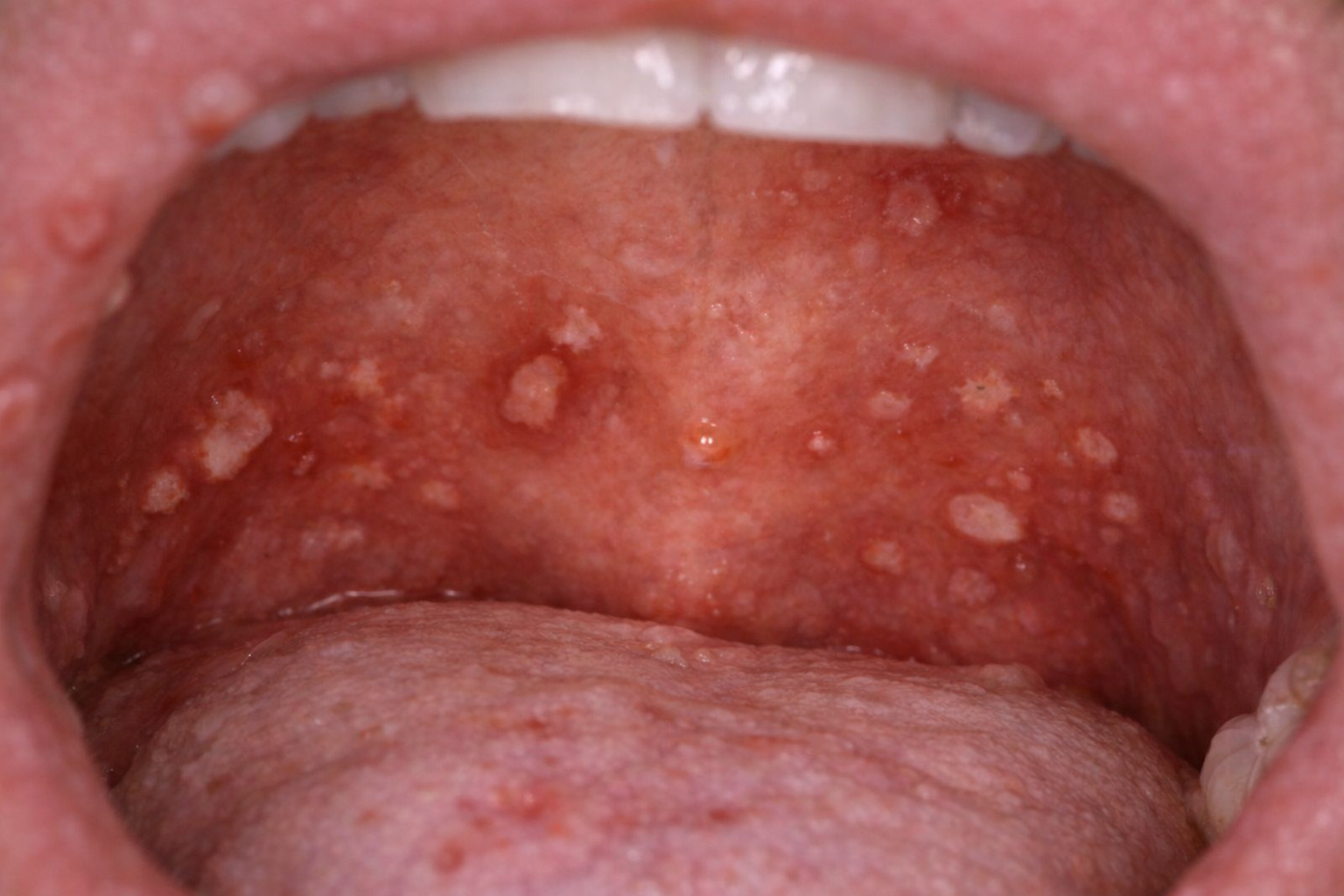
Can You Get an STD in Your Throat?
Yes, you can. This is one of the most overlooked parts of the conversation. Oral sex can lead to throat infections caused by:
- Gonorrhoea
- Chlamydia
- Syphilis
- Herpes
- HPV
The difficulty is that throat symptoms are often mild. Some people assume it is just irritation or a normal sore throat. Others have no symptoms at all. That is why oral STDs can be missed unless proper testing is done.
Can You Get an STD From Receiving Oral Sex?
Yes. People often focus only on the person giving oral sex, but receiving oral sex can also carry risks. For example:
- A partner with oral herpes can transmit genital herpes
- Oral syphilis or oral gonorrhoea can spread to the genitals
If a partner has cold sores, mouth ulcers, or any unusual symptoms around the mouth, it is safer to avoid sexual contact until the cause is clear.
Why Oral Sex Risk Is Often Underestimated
A lot of people think of oral sex as “low risk” and stop the conversation there. The problem is that low risk is not the same as no risk. Several things can increase the chance of transmission:
- Multiple sexual partners
- No condom or dental dam use
- Existing genital sores
- Poor oral health
- Bleeding gums
- A weakened immune system
Another major reason risk is underestimated is that many infections cause no symptoms in the beginning. A person can feel completely fine and still pass an infection to someone else.
How to Reduce the Risk
No method is perfect, but several practical steps can lower the risk quite a bit.
1. Use Protection
Using a condom during oral sex on a penis and a dental dam during oral-vaginal or oral-anal contact reduces exposure to infected fluids and skin. It may not remove all risk, but it does lower it.
2. Avoid Oral Sex During Active Outbreaks
If you or your partner has cold sores, genital ulcers, unexplained discharge, rash, or irritation, it is better to avoid sexual contact until the situation has been checked. This matters because active lesions often carry a higher chance of transmission.
3. Maintain Good Oral Health
The mouth is part of the risk equation. Bleeding gums, mouth ulcers, and recent dental procedures can create easier entry points for infection. Good oral hygiene will not eliminate the risk, but it helps reduce it.
4. Get Vaccinated
Vaccines are available for HPV and Hepatitis B. These are among the most effective preventive tools available and should not be overlooked.
5. Routine STD Screening
Routine screening is important, especially if you have:
- A new partner
- Multiple partners
- Unprotected sex
- Suspicious symptoms
If oral exposure has occurred, throat swabs may be recommended because some infections will not show up clearly from symptoms alone.
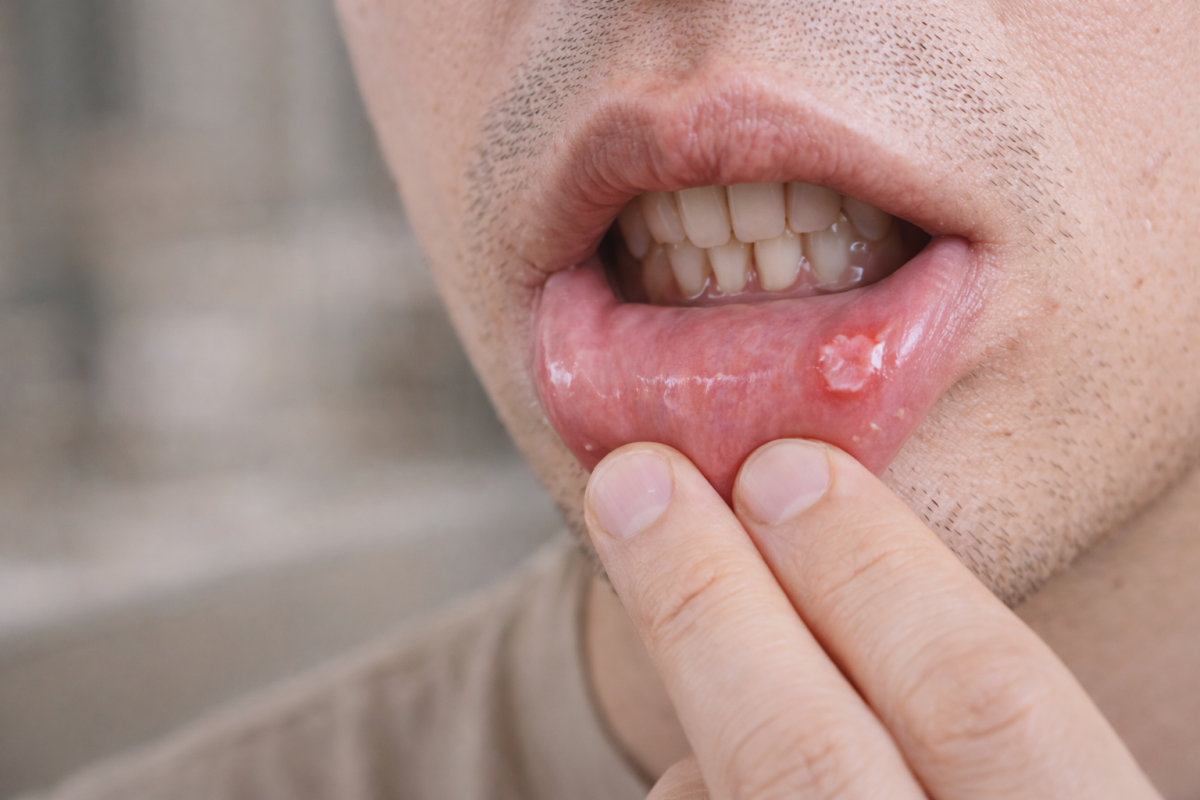
What Are the Symptoms of Oral STDs?
Symptoms vary depending on the infection. Some people notice almost nothing, while others develop more obvious problems. Possible signs include:
- Sore throat
- Pain when swallowing
- Mouth ulcers
- Swollen glands
- White patches in the throat
- No symptoms at all
The last point is important. No symptoms do not always mean no infection.
When Should You See a Doctor?
You should get checked if you notice:
- A sore throat that does not settle after sexual exposure
- Mouth ulcers that do not heal
- Genital symptoms after oral contact
- Known exposure to a partner diagnosed with an STD
The earlier the cause is identified, the easier it usually is to manage.
Why Early Diagnosis Matters
Many oral STDs respond well to early treatment. Bacterial infections such as gonorrhoea, chlamydia, and syphilis can usually be treated effectively with antibiotics. Viral infections like herpes are managed rather than cured, but treatment can still reduce symptoms and lower the chance of passing the virus on. Getting checked early can:
- Shorten the duration of symptoms
- Reduce transmission
- Lower the risk of complications
- Provide reassurance
Delaying care can mean the infection continues silently.
Final Thoughts: Is Oral Sex Safe?
Oral sex is generally lower risk than some other forms of sexual activity, but it is not completely safe. STDs can still spread through oral-genital and oral-anal contact, even when no one notices symptoms.
That does not mean people need to panic. It simply means it is better to make informed choices. Barrier protection, vaccination, regular testing, and honest communication with partners all matter.
If you are concerned about possible exposure or you have symptoms that do not feel normal, it is worth getting checked rather than guessing. Dr Chong Clinic provides confidential STD screening, medical consultation, and treatment in a discreet setting.
Frequently Asked Questions (FAQs)
1. Can you get an STD from oral sex even if there is no ejaculation?
Yes. Many STDs can spread through skin contact, pre-ejaculatory fluid, and other secretions. Ejaculation is not necessary for transmission.
2. Are oral STDs less serious than genital STDs?
Not always. Some oral infections are mild, but others can still cause complications or be passed to other partners if not treated.
3. How soon should I get tested after oral sex exposure?
It depends on the infection. In many cases, testing after 1 to 2 weeks may be considered, but timing varies. A doctor can advise based on the specific exposure.
4. Can using mouthwash after oral sex prevent STDs?
No. Mouthwash is not a reliable way to prevent STD transmission. Protection, vaccination, and proper testing are far more important.
*All images used in this article are AI-generated.